Stepping into an operating room for the first time may seem daunting, but it doesn’t have to be! You already have all of the technical knowledge necessary to prepare an operating room successfully, but there are some nuances that you don’t want to forget.
Read MoreCathy Barnette

Recent Posts
Video: How to Prepare for the O.R.
Top 3 Cardiac Medications for Small Animal Vet Techs

![]() As you have likely noticed in your pharmacology courses, there is a long list of cardiac medications that can be used to treat a wide variety of cardiac conditions.
As you have likely noticed in your pharmacology courses, there is a long list of cardiac medications that can be used to treat a wide variety of cardiac conditions.
If you find yourself working in veterinary cardiology, you will likely become familiar with many of these medications.
If you opt to work in general practice, though, you really only need to be highly familiar with a handful of cardiac medications. While you may occasionally encounter patients taking other medications, it will likely be rare enough that you can consult a reference as needed.
Read MoreControlled Drug Logs: FAQs for Vet Techs

![]() While controlled drug logs are primarily the responsibility of the veterinarian (after all, it’s their DEA license that’s associated with the controlled drug box), many vet techs also play a role in logging controlled drugs.
While controlled drug logs are primarily the responsibility of the veterinarian (after all, it’s their DEA license that’s associated with the controlled drug box), many vet techs also play a role in logging controlled drugs.
If your responsibilities include anesthesia and/or surgery, you will likely be handling controlled drugs on a regular basis, and you will need to log them accordingly.
Read MoreTracing the Flow of Blood Through the Heart: A Summary for Vet Techs
They say a picture is worth a thousand words, so here’s a helpful image:
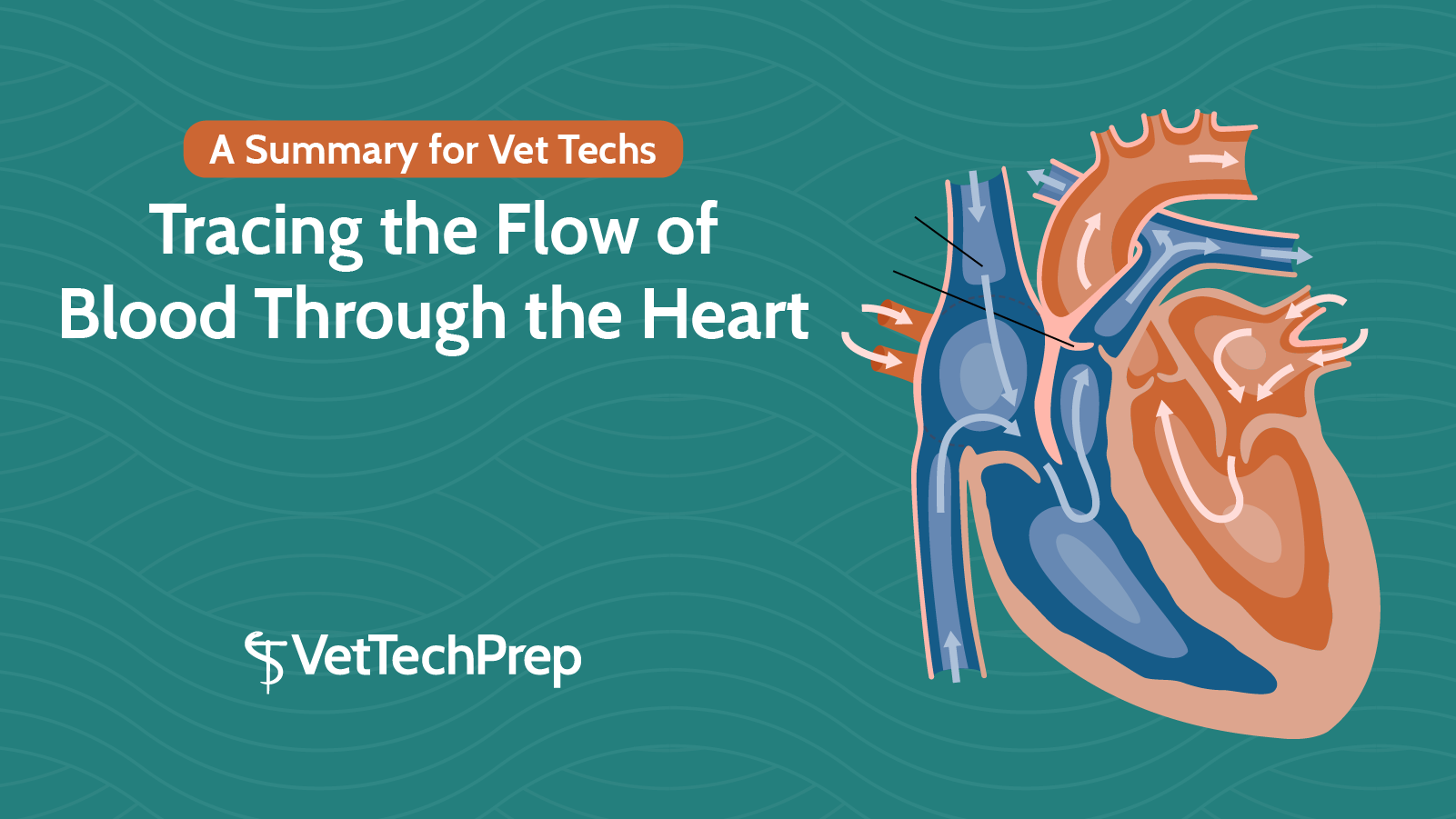
 This particular image is relatively useless at first glance, because it contains a lot of information. If you take the time to actually trace the flow of blood through the heart, however, it can be very helpful!
This particular image is relatively useless at first glance, because it contains a lot of information. If you take the time to actually trace the flow of blood through the heart, however, it can be very helpful!
Medical Math for Vet Techs: A Lidocaine CRI Case Study

A 9 yo MN mixed breed dog, weighing 72 pounds (32.7 kg), presented for a recent onset of panting, shortness of breath, weakness, and episodes of syncope. On physical examination, the dog’s heart rate was 160 bpm, his mucous membranes were pale, and his pulses were weak and thready. An ECG was immediately performed. On the ECG, the veterinarian noted an absence of P waves accompanied by wide and bizarre QRS complexes. Based on the ECG findings, the dog was diagnosed with ventricular tachycardia.
Read MoreImproving Client Compliance: Dentistry Tips for Vet Techs

![]() As a vet tech working in general practice, you will probably discuss dental care with nearly all of your patients.
As a vet tech working in general practice, you will probably discuss dental care with nearly all of your patients.
Whether you’re recommending home care to a new puppy owner, recommending a dental cleaning to the owner of a middle-aged pet, or calling a client during their pet’s dental procedure to recommend extractions, it’s important to be comfortable making recommendations in a way that improves client compliance.
Read MoreVet Tech Case Study: Eosinophilic Granuloma Complex

![]() Pepper, a 3 yo FS DSH, presents on a busy Friday afternoon for a recent history of skin irritation and licking. She is an indoor/outdoor cat and is up-to-date on FVRCP, Rabies, and FeLV vaccines, but not much is known about her medical history.
Pepper, a 3 yo FS DSH, presents on a busy Friday afternoon for a recent history of skin irritation and licking. She is an indoor/outdoor cat and is up-to-date on FVRCP, Rabies, and FeLV vaccines, but not much is known about her medical history.
She was adopted from a shelter just a few months earlier. Pepper’s owner reports that she tries to give Revolution® monthly, though she has missed a few doses; Pepper’s most recent dose was administered roughly five weeks ago.
Read MoreThe Vet Tech’s Role in Managing Rodenticide Toxicity

 When you hear the phrase “rodenticide toxicity,” what’s the first type of toxicity that comes to mind? If you’re like most people, you probably think of anticoagulant rodenticides.
When you hear the phrase “rodenticide toxicity,” what’s the first type of toxicity that comes to mind? If you’re like most people, you probably think of anticoagulant rodenticides.
However, there are a variety of different rodenticides that can have toxic effects on pets. As a vet tech, it’s important for you to be familiar with these toxins and know your role in managing possible rodenticide toxicity.
Read MoreHandling Client Calls About Possible Toxicities: 5 Tips for Vet Techs

![]() Clients and non-clients alike often call veterinary clinics about possible toxicity concerns. In most cases, the receptionists answer these calls and then forward them to a vet tech for evaluation.
Clients and non-clients alike often call veterinary clinics about possible toxicity concerns. In most cases, the receptionists answer these calls and then forward them to a vet tech for evaluation.
Your job, as the vet tech, is to triage the client’s concern and determine whether the pet needs veterinary care. In some cases, it will be obvious that the client’s concern is unfounded and the item that the pet ate does not pose a risk. In other cases, however, the correct solution will not be so clear.
When in doubt, you can always ask the veterinarian for a recommendation.
Read MoreHow Much Damage Can a Few Grapes Cause? A Grape Toxicity Case Study for Vet Techs

 You are working a busy day as a vet tech in small animal general practice when a receptionist pages back to the treatment area.
You are working a busy day as a vet tech in small animal general practice when a receptionist pages back to the treatment area.
Mrs. Jones, a longtime client, is on the phone. She is concerned because her dog, Maximus, may have just eaten several grapes out of the trash can. Maximus is a 6 yo Miniature Pinscher and, according to your medical records, he weighs about 13 lbs.
How concerned should Mrs. Jones be? What should you tell her to do?
Read MoreTips for Tackling the TPR

 As a vet tech, one of your many responsibilities will be helping the veterinarian see appointments. In many cases, you will be the first to enter the exam room, in order to obtain the patient’s history, assess the TPR, and perform a brief triage exam.
As a vet tech, one of your many responsibilities will be helping the veterinarian see appointments. In many cases, you will be the first to enter the exam room, in order to obtain the patient’s history, assess the TPR, and perform a brief triage exam.
Since this is a routine that you will be performing nearly every day, it makes sense to give some thought to how to do it correctly!
Read MoreFocus on the Medical History: 5 Tips for Vet Techs

As a vet tech, you will often be the first person who enters an exam room with the client and patient. In addition to assessing the pet’s TPR (temperature, pulse, and respiration) and performing a brief triage exam, you will also need to collect a preliminary medical history.
While the triage exam and TPR are important, the history is often even more valuable. Therefore, it’s important to resist the temptation to rush through it!
Read MoreTop 5 Myths About Veterinary Chemotherapy

![]() When a pet is diagnosed with cancer and the word chemotherapy is mentioned, clients often jump to a number of conclusions.
When a pet is diagnosed with cancer and the word chemotherapy is mentioned, clients often jump to a number of conclusions.
Many of these conclusions are based on what clients have seen or heard in the field of human chemotherapy.
While drawing comparisons between human and veterinary chemotherapy is completely natural and understandable, many of these comparisons are not true; these preconceptions may prevent clients from considering chemotherapy with an open mind.
Read MoreCan You Hear Me Now?! Protect Your Hearing While Working as a Vet Tech

![]() Barking dogs are loud; there’s no doubt about that! Whether your practice includes a large-scale boarding facility or only contains a few kennels to house surgical and hospitalized patients, every practice has areas that become noisy at times.
Barking dogs are loud; there’s no doubt about that! Whether your practice includes a large-scale boarding facility or only contains a few kennels to house surgical and hospitalized patients, every practice has areas that become noisy at times.
Any time you have dogs barking in a confined area, especially when surrounded by concrete, stainless steel, and other surfaces that don’t absorb sound very well, you can expect large amounts of noise.
Read MoreWho is More Likely to be Injured at Work: A Firefighter or a Vet Tech?

According to 2016 statistics, someone working full-time in the veterinary field has a 12% chance of sustaining a work-related injury or illness in any given year.1 This means that veterinary professionals are more likely to be injured at work than almost any other career, with the sole exception of residential care nursing!2
While firefighting may seem more hazardous at first glance, and firefighting injuries are probably more likely to be serious or fatal than veterinary injuries, firefighters have a 9.5% likelihood of being injured at work in any given year,2 which means they are 20% less likely to be injured at work in a given year than a full-time veterinary worker.
Read More
